

放射性肺损伤(Radiation-induced lung injury, RILI)是胸部恶性肿瘤(肺癌、食管癌、乳腺癌、纵膈内恶性肿瘤)在接受放射性治疗过程中正常肺组织不可避免的受到一定剂量的射线照射而造成的肺损伤[1]。放射性肺损伤作为临床上常见的放疗并发症,影响着肿瘤靶区剂量以及全局放疗的疗效,是放疗疗效最大程度发挥的主要制约因素。
放射性肺损伤分为早期的急性放射性肺炎和晚期的慢性放射性肺纤维化,早期组织损伤表现为,上皮或内皮细胞释放炎症介质促进凝血并使 ECM 短暂增加,同时促进血管扩张和通透性增加。招募炎症细胞到达损伤部位,随后炎症细胞可分泌多种细胞因子,增强炎症反应并促进纤维细胞增殖。
肺纤维化是晚期的损伤改变,其病理改变主要表现为上皮细胞受损、肺部细胞外基质的积聚增加和胶原纤维增生等,持续发展可导致肺组织结构破坏,肺换气功能受损,呼吸衰竭,严重威胁人类的生命健康[2, 3]。纤维化通常被认为是一种损伤后修复失控的伤口愈合反应。因此在肺损伤修复过程中,有四个不同的阶段,包括(1)凝血阶段;(2)炎症阶段;(3)成纤维细胞迁移和增殖阶段;(4)恢复正常组织结构的重塑阶段[4]。

辐射所致肺损伤[5] (A) 健康肺泡;(B) 放射性肺炎;(B) 放射性肺纤维
派思维新放射性肺炎经典模型案例一
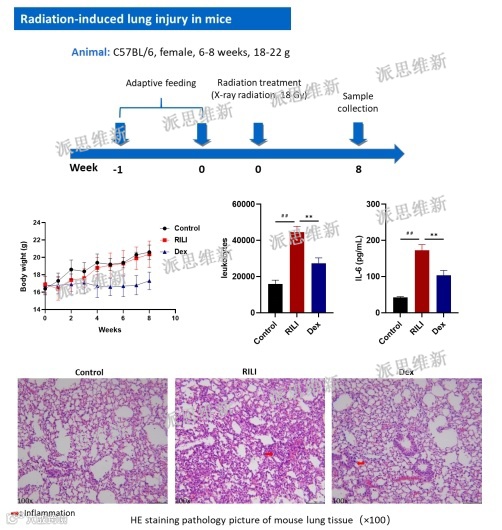
派思维新放射性肺炎经典模型案例二


派思维新急性全身放射性疾病动物模型案例


放射性肠炎机制[17]
派思维新放射性肠炎经典模型案例

急性放射性皮肤损伤(RSI)常发生于核事故和肿瘤放射治疗中。放射治疗所致的皮肤损伤多为亚急性,以Ⅰ~Ⅱ度放射性皮肤损伤常见,Ⅲ 度及以上放射性皮肤损伤多由事故性照射引起。在肿瘤放疗中,RSIs的发生率也逐渐升高,近85%的肿瘤患者因放疗而出现不同程度的皮肤损伤[18]。研究发现,约95%的患者在接受放疗或放疗后都会出现皮肤红肿,甚至溃疡,且常伴有脱发脱屑,这说明放射性皮肤损伤是最为常见放射治疗并发症之一。与普通烧伤和溃疡不同,辐射直接损害皮肤及其深层组织细胞,导致受辐射区域干燥、失去弹性、色素沉着、软组织纤维化、毛细血管扩张和放射性皮炎[19]。急性放射性皮肤损伤患者临床主要表现为局部皮肤瘙痒,会发生脱皮、疼痛、溃疡造成局部感染;病情严重的患者皮肤会变薄,产生瘢痕、挛缩[20,21],严重影响患者的生活质量。

放射性皮肤损伤机制[22]
派思维新放射性皮炎经典模型案例
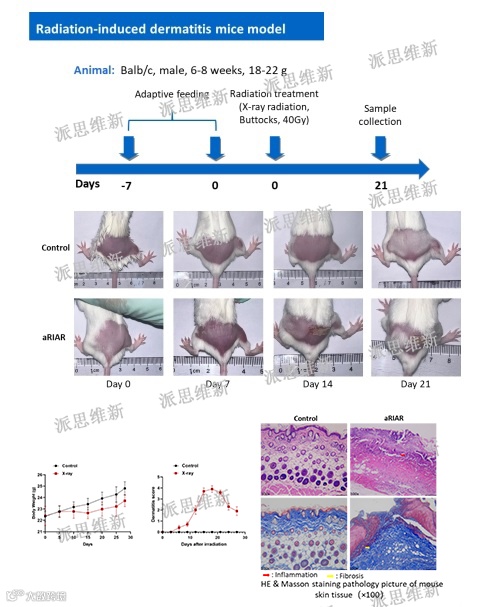
Novopathway


- 上下滑动查看参考资料 -
[1] JENKINS P, WELSH A. Computed tomography appearance of early radiation injury to the lung: Correlation with clinical and dosimetric factors [J]. Int J Radiat Oncol Biol Phys, 2011, 81(1): 97.
[2] Chargari C, Riet F, Mazevet M, et al. Complications of thoracic radiotherapy[J]. La Presse Médicale, 2013,42(9): e342-e351.
[3] Lierova A, Jelicova M, Nemcova M, et al. Cytokines and radiation-induced pulmonary injuries[J]. Journal of Radiation Research, 2018,59(6):709-753.
[4] Wynn T A. Integrating mechanisms of pulmonary fibrosis[J]. The Journal of Experimental Medicine, 2011,208(7):1339-1350.
[5] Jin H, Yoo Y, Kim Y, Kim Y, Cho J, Lee YS. Radiation-Induced Lung Fibrosis: Preclinical Animal Models and Therapeutic Strategies. Cancers (Basel). 2020 Jun 12;12(6):1561.
[6] FDA. Biologic license application: 125031. NEULASTA. 2015. Label ( PDF) [EB/OL]. Silver Spring: FDA. 2015-11-13[2021-02-22]. https://www. accessdata. fda. gov /drugsatfda_ docs/label /2015 /125031s180lbl. pdf.
[7] FDA. Biologic license application: 103353. NEUPOGEN. 2015. Label (PDF) [EB/OL]. Silver Spring: FDA. 2015- 03-30[2021-02-22[. https://www. accessdata. fda. Gov/drugsatfda_ docs/label /2016 /103353s5188. pdf.
[8] FDA. Biologic license application: 103362. LEUKINE. 2018. Label ( PDF) [EB/OL]. Silver Spring:
[9] FDA. 2018-03-29[2021-02-22]. https://www. accessdata. fda. gov /drugsatfda_ docs/label /2018 /103362s5240lbl. pdf.
[10] FDA. Biologic license application: 125268. NPLATE. 2021. Lable ( PDF) [EB /OL]. Silver Spring:
[11] FDA. 2021- 01-28[2021-02-22]. https://www. accessdata. fda. gov /drugsatfda _ docs/label /2021 /125268s168lbl. pdf.
[12] Singh VK, Newman VL, Berg AN, MacVittie TJ. Animal models for acute radiation syndrome drug discovery. Expert Opin Drug Discov. 2015 May;10 (5):497-517.
[13] Hauerjensen M, Denham JW, Andreyev HJN. Radiation enteropathy-pathogenesis, treatment and prevention[J]. Nat Rev Gastroenterol Hepatol, 2014,11(10):470-479.
[14] Theis VS, Sripadam R, Ramani V, et al. Chronic radiation enteritis[J]. Clin Oncol (R Coll Radiol), 2010,22(1):70-83
[15] KUMAGAI T, RAHMAN F, SMITH A M. The microbiome and radiation induced-bowel injury: evidence for potential mechanistic role in disease pathogenesis [J]. Nutrients,2018,10( 10) : 1405.
[16] HARB A H, ABOUT F C, SHARARA A I. Radiation enteritis [J]. Current Gastroenterology Reports, 2014, 16( 5) : 1-9.
[17] Fan J, Lin B, Fan M, et al. Research progress on the mechanism of radiation enteritis.Front Oncol. 2022;12:888962. Published 2022 Sep 5. doi:10.3389/fonc.2022.888962.
[18] Salvo N, Barnes E, van Draanen J, et al. Prophylaxis and management of acute radiation-induced skin reactions: a systematic review of the literature.Curr Oncol. 2010;17(4):94-112. doi:10.3747/co.v17i4.493.
[19] Singh M, Alavi A, Wong R, Akita S. Radiodermatitis: A Review of Our Current Understanding.Am J Clin Dermatol. 2016;17(3):277-292. doi:10.1007/s40257-016-0186-4.
[20] KumarSoniS, Basu M, AgrawalP, etal. Evaluation of gammar adiation induced biochemical changes skin for dose assesment: a study on small experimental animals [J]. Disaster Med Public Health Prep, 2019, 13 (2): 197- 202.
[21] AdamsT G, YeddanapudiN, Clay M, etal. Modeling cutaneous radiation injure from fallout [J]. Disaster Med Public Health Prep, 2019,13 (3): 463-469
[22] Yang X, Ren H, Guo X, Hu C, Fu J. Radiation-induced skin injury: pathogenesis, treatment, and management.Aging (Albany NY). 2020;12(22):23379-23393. doi:10.18632/aging.103932.
部分图文信息汇总于专业期刊,如有错误欢迎指正!


